How Navigators support people who contact Palliative Care Connect
An article written by Amber Bisset, Mariana Ricci and Kate Swetenham, SA Health
Last week, we introduced palliative care navigation and the role of Palliative Care Connect (PCC). This week, we’re looking at what happens when someone contacts PCC, why they reach out, and how PCC Navigators help them understand options and move forward with confidence.
PCC is a free statewide service providing information, service linkages and supports for people living with a life-limiting illness, and their family, friends and carers. It’s also available to health, aged care, disability and community service professionals seeking assistance for their clients. PCC Navigators - experienced nurses and social workers - listen, interpret what’s happening and talk through practical next steps. The examples below show the kinds of support delivered by PCC that people find helpful.
When and why people reach out:
People contact PCC for many reasons, including when they want to:
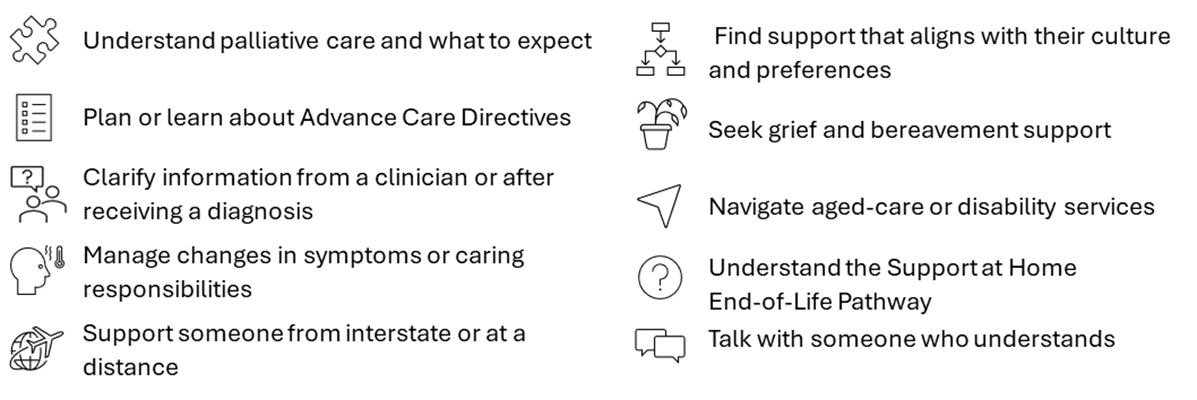
Whatever the reason, speaking with someone who listens and offers clear next steps often brings clarity and relief.
What navigation looks like in practice
A family in crisis about provision of end-of-life care in an aged care home: After being told their loved one was at end of life, the family called PCC unsure whether the aged care home could meet his needs. A PCC Navigator explained how the care he was receiving aligned with his dementia and end-of-life needs and guided them on which questions to raise with staff. Their worry eased, as they were better informed, and able to focus on time together.
A daughter navigating system barriers in remote South Australia: Her mother’s rapid decline and limited local services meant assessments for higher level supports were delayed or unavailable. Exhausted from repeating her story and getting nowhere, she contacted PCC. A PCC Navigator listened, clarified what was realistic, followed up with key contacts and provided written information she could revisit. While system barriers remained, she was able to resolve some of the issues and felt more supported and less alone through the caring process.
What we're hearing from callers
People often tell us that having time to talk things through with a PCC Navigator helps them feel heard and supported. They value the practical guidance - who to call, what to ask and how services fit together - as well as having written information to return to. People frequently describe feeling less stressed and more able to understand the issues they are facing, with a plan to move forward.
“Everything was done in a way that I felt reassured and not alone in dealing with this. Couldn’t have asked for better support.”
“The calm and honest advice provided by the Navigator was most appreciated. It reduced my stress in this difficult time.”
“PCC has been the glue that has held everything together through a very difficult time.”
You don't have to work it out alone
PCC is free, interpreter supported, and no referral is needed. You can call for yourself or someone you’re supporting.
Call 1800 725 548 (PALLI8) or visit www.palliativecareconnect.com.au.
Next, we’ll look at how PCC Navigators support health, aged care and community professionals by clarifying pathways, providing consistent information and helping families navigate care.
Authors

Amber Bisset
Project Officer, Health Services Programs
Clinical System Support and Improvement, SA Health

Mariana Ricci
Manager – End of Life Care, Health Services Programs
Clinical System Support and Improvement, SA Health

Kate Swetenham
Director of Nursing - End of Life Care, Health Services Programs
Clinical System Support and Improvement, SA Health